The Gut-Thyroid Connection
The Gut-Thyroid Connection
The Gut-Thyroid Connection is well researched, with a strong interrelated connection present between the thyroid and gut. Hippocrates said: “All disease begins in the gut.” 2,500 years later we’re just beginning to understand how right he was.[1] In this article we will explore the Gut-Thyroid Connection, also known as the Gut-Thyroid Axis. Thyroid and gut diseases often co-exist, for example, autoimmune thyroid disease and celiac disease often show up together. The link has been known about since the 1950’s but it’s just gaining traction now. But first, what exactly does your thyroid do?
What is the Thyroid Gland?
The thyroid is a butterfly-shaped endocrine gland, which is situated at the front of the throat, below the larynx (the Voice Box / Adam’s apple). The two lobes lie on either side of the windpipe.
The thyroid’s job is to make thyroid hormones, which are secreted into the blood and then carried around the body. Thyroid hormones help the body use energy, stay warm and keep the brain, heart, muscles, and other organs working as they should. [2]
The thyroid regulates the body’s metabolic processes, influences digestion, heart, mood, brain development and muscle control. There are a number of conditions that affect the thyroid. Nutrient deficiencies and autoimmunity play a big part, as these are often triggered from long standing gut problems. [3]
Thyroid Conditions
- Goiter: A general term for thyroid swelling. Goiters can be harmless, or can represent iodine deficiency or a condition associated with thyroid inflammation called Hashimoto’s thyroiditis.
- Thyroiditis: Inflammation of the thyroid, usually from a viral infection or autoimmune condition. Thyroiditis can be painful, or have no symptoms at all.
- Hyperthyroidism: Excessive thyroid hormone production. Hyperthyroidism is most often caused by Graves disease or an overactive thyroid nodule.
- Hypothyroidism: Low production of thyroid hormone. Thyroid damage caused by autoimmune disease is the most common cause of hypothyroidism .
- Graves disease: An autoimmune condition in which the thyroid is overstimulated, causing hyperthyroidism.
- Thyroid cancer: An uncommon form of cancer, thyroid cancer is usually curable. Surgery, radiation, and hormone treatments may be used to treat thyroid cancer.
- Thyroid nodule: A small abnormal mass or lump in the thyroid gland. Thyroid nodules are extremely common. Few are cancerous. They may secrete excess hormones, causing hyperthyroidism, or cause no problems.
- Thyroid storm: A rare form of hyperthyroidism in which extremely high thyroid hormone levels cause severe illness. [4]
What is the gut?
When we talk about the gut, we are mainly referring to your small and large intestine. The large intestine houses most of your gut bacteria. Your gut is supported by your stomach, liver, pancreas and gallbladder. [5]
What does it do?
Your gut has many functions, but the key ones are:
- houses the majority of your microbiome
- digests and absorbs nutrients
- supports immune function (approximately 70%)
- plays a role in producing chemicals that affect how we feel
Gut microbiome
There are trillions of microbes, their functions and genes (including bacteria, yeast, fungi and parasites) and their genetic material living within the gut. There are more than 1,000 species that have been identified.
Gut Microbiota: The types of organisms (bacteria, viruses, parasites etc.) present in your gut. The terms ‘microbiota’ or ‘microflora’ are used interchangeably. Diet, medication, environment and genes are just some of the factors that can influence your gut microbiota.[6]
What does it do?
Gut microbes do various things, these include:
- Produce vitamins, including vitamin K and B vitamins
- Produces short chain fatty acids, which fuel your gut cells
- Supports immune function and defends against pathogens
- Influence how often you go to the toilet
- Regulates health of gut
- Ferments fibre that your body cannot digest
- Influences mood and mental health
- Influences sleep
- Supports hormone regulation
- Regulates metabolism
Gut Dysbiosis
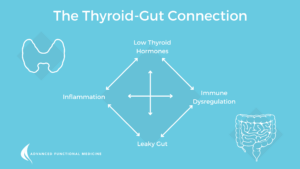
Dysbiosis refers to a condition where microbial flora (gut microbiota) in the gut imbalanced. If our gut microbiota is in a state of dysbiosis, it’ll negatively affect different aspects of our health, including our immune system, physical and mental health. These imbalances have been associated with different illnesses, like inflammatory bowel disease, chronic fatigue syndrome and thyroid diseases such as Hashimoto’s thyroiditis and Graves’ disease. A leaky bowel wall leads to bacteria and endotoxins building up in the bloodstream creating an immune response. This is an important stimulus for inflammatory cytokine activation. Poor gut health may impair thyroid function and poor thyroid function can contribute to inflammation and ‘leaky gut’. [7]
The Gut-Thyroid Connection
Our thyroid hormones play a key role in things like our ability to conceive, our sleep patterns, our mental health, our energy levels, and how well we digest, assimilate, and absorb our food and nutrients. That’s because thyroid hormones like thyroxine (T4) and triiodothyronine (T3) define basal metabolism throughout the entire body, particularly in the intestine and internal organs.[8]
The fact that thyroid and digestive issues often coexist has been well researched and documented [9], and the liver is the most affected organ in both hyperthyroidism and hypothyroidism.[10] The gastrointestinal manifestations of thyroid disease are generally due to reduced motility in hypothyroidism, increased motility in hyperthyroidism, autoimmune gastritis, or oesophageal compression by a thyroid process. [9]
Gastrointestinal symptoms of thyroid dysfunction are numerous, and include trouble swallowing, heartburn, indigestion, reduced acid production, nausea or vomiting, gallbladder complaints, abdominal discomfort, gas, bloating, diarrhea, constipation, and general digestive complaints including Irritable Bowel Syndrome (IBS).[11]
It’s also been well-documented that an imbalance in gut bacteria/gut infections can affect the thyroid; so the connection works both ways. The result can be a perpetual cycle as one issue exacerbates another, and vice-versa. “The gut-thyroid connection can be a vicious circle as hypothyroidism causes poor digestive health, and poor digestive health may cause the treatment of hypothyroidism to not be as effective,” says Dr. Akhunji. [12]
Examples:
The Gut-Thyroid Connection in relation to Hyperthyroidism: ”Excessive thyroid function, or hyperthyroid, can be associated with diarrhoea, hyper-defecation, and malabsorption. It can also include trouble swallowing due to an enlarged thyroid gland and abnormal liver function tests” Dr. Bulsiewicz. [12]
The Gut-Thyroid Connection in relation to Hypothyroidism: “Without enough thyroid hormones, many of the body’s functions slow down,” says Dr. Akhunji. [12] “In a normal digestive tract, the muscles lining the small intestine and large intestine contract, which helps to move digested food down the intestines. In the case of hypothyroidism, the contraction is slowed down. In addition to the slow digestive process, the elimination of stool also slows down.”
The gut-thyroid-immune connection
An important function of the gut is that it plays host to 70% of the immune tissue in the body. This portion of the immune system is referred to as gut-associated lymphoid tissue or GALT for short. The GALT is made up of several types of lymphoid tissues that store immune cells, such as T & B lymphocytes, that carry out attacks and produce antibodies against antigens, molecules recognised by the immune system as potential threats. [1]
Problems occur when either of these protective functions of the gut are compromised. If the intestinal barrier becomes permeable (i.e. “leaky gut”), large protein molecules escape into the bloodstream. Since these proteins don’t belong outside of the gut, the body mounts an immune response and attacks them. Studies show that these attacks play a role in the development of autoimmune diseases [13] such as Hashimoto’s. [1]
The gut-bacteria-thyroid connection
Gut dysbiosis significantly reduces [14] the conversion of T3S and T3AC to T3. This is one of the reasons why people with poor gut function may have thyroid symptoms but normal test results.
Inflammation in the gut also reduces T3 by raising cortisol. Cortisol decreases active T3 levels while increasing levels of inactive T3. [1]
Studies have also shown [1] that cell walls of intestinal bacteria, called lipopolysaccharides (LPS), negatively effect thyroid metabolism in several ways. LPS:
- reduce thyroid hormone levels;
- dull thyroid hormone receptor sites;
- increase amounts of inactive T3;
- decrease TSH; and
- promote autoimmune thyroid disease (AITD).
Here are a few other ways your gut and thyroid are linked:
Nutrients
The state of your gut and its microbes can also influence the absorption of micronutrients like iodine, iron and copper, which you need for thyroid health. Your microbes have the ability to increase the bioavailability of iron in the gut by producing short chain fatty acids. Your gut microbes also regulate how much iodine you use and how it is broken down and circulated in the body. Iodine is essential for thyroid health. Inflammatory bowel disease can also impair iodine absorption. [5]
Stress
When we are stressed, we produce more cortisol (stress hormone), which may reduce the amount T3 (the active thyroid hormone). Stress comes in all shapes and sizes, perceived or actual, but one source is your gut. Inflammation in your gut, whether through dysbiosis, [5] immune response or gastrointestinal disease, will increase circulating cortisol, which if prolonged can have a negative effect on T3 levels.
Immune system
The gut is home to 70% of the immune system in the form of gut associated lymphoid tissue (known as GALT). GALT acts like a larder for storing part of the immune system’s defence system, immune cells. Immune cells, like T and B lymphocytes are deployed to defend against potential threats and in the case of Hashimoto’s, immune cells attack self. [5]
But what does this mean in relation to thyroid health? Your immune system can be triggered through something going on in your gut, take leaky gut, stuff can get through that shouldn’t and so your body amounts an immune response. If a thyroid condition has your immune system working overtime, this can have a negative effect on your gut health.
Converting hormones into the useful ones
Some T4 gets converted into the active T3 in the gut using an enzyme, intestinal sulfatase which comes from the gut’s beneficial microbes. [5] If the gut is out of whack (dysbiosis), it can reduce the conversion of the inactive T4 to the active T3.
Constipation
Low thyroid function can slow down how often you need to go. Transit time is linked with diversity of gut microbes. Constipation comes with its own issues, in particular, the effect on circulating oestrogen levels, which may affect fertility and menopausal symptoms. [5]
Gallbladder
The gall bladder stores bile. Bile is important as it regulates metabolism through changes in thyroid hormones and helps to digest and absorb fats. Research shows that those with hypothyroidism had reduced bile acids levels. Insufficient bile can impair how well you digest and absorb nutrients and how well your body deals with hormones and toxins that it needs to get rid of. [5]
Probiotics
Research indicates that specific probiotics may be beneficial on thyroid hormone and function and the availability of minerals. [5]
Finally,
One thing to keep in mind is that just because you have a gut issue doesn’t automatically mean you also have a thyroid issue. However, if you’re struggling with digestive symptoms, or symptoms of thyroid disorders, be sure to get your thyroid levels tested.
Our practitioners make sure we investigate both the underlying causes and imbalances to ensure you get the best tailored approach.
Contact us to find out more.